Solutions
Platform
Healthcare AI
© Copyright 2026 Aidoc
Explore how Aidoc’s clinical AI solutions can increase hospital efficiency, show proven return on investment, and help enable better outcomes.
Learn more →Prioritize findings and activate care teams in streamlined workflows
Consistently measure disease and capture incidental findings
Setting the standard for neuro care with real time notification
Streamline workflows and centralize patient management
Discover how Aidoc’s AI platform offers seamless end-to-end integration into a facility’s existing IT infrastructure enabling implementation of AI at scale.
Learn more →Aidoc’s proprietary enterprise platform
Connect the right users across workflows
Ensure patients are identified, captured and followed
Custom configuration with minimal IT lift
Vetted third-party algorithm developers and OEMs
Information and resources about AI transformation rooted in real-world experiences.
Learn More →Go beyond algorithms to build a scalable AI strategy.
A framework to integrate AI into clinical practice.
A new approach to clinical AI, powered by Aidoc’s CARE™.
Learn more about Aidoc’s approach, mission and leadership team that is revolutionizing healthcare with AI.
Learn more →Explore how Aidoc’s clinical AI solutions can increase hospital efficiency, show proven return on investment, and help enable better outcomes.
Learn more →Prioritize findings and activate care teams in streamlined workflows
Consistently measure disease and capture incidental findings
Setting the standard for neuro care with real time notification
Streamline workflows and centralize patient management
Discover how Aidoc’s AI platform offers seamless end-to-end integration into a facility’s existing IT infrastructure enabling implementation of AI at scale.
Learn more →Aidoc’s proprietary enterprise platform
Connect the right users across workflows
Ensure patients are identified, captured and followed
Custom configuration with minimal IT lift
Vetted third-party algorithm developers and OEMs
Information and resources about AI transformation rooted in real-world experiences.
Learn More →Go beyond algorithms to build a scalable AI strategy.
A framework to integrate AI into clinical practice.
A new approach to clinical AI, powered by Aidoc’s CARE™.
Learn more about Aidoc’s approach, mission and leadership team that is revolutionizing healthcare with AI.
Learn more →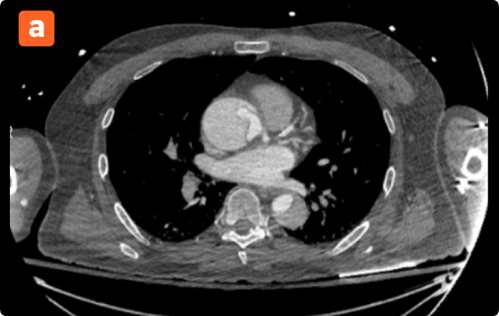
Radiology: Helps triage urgent cardiovascular cases, resulting in more timely notifications to specialists. Findings are validated by a radiologist first to enhance hub-spoke models while preventing unnecessary alerts.
Mobile app providing real-time notification of time-sensitive cases, built-in risk stratification* and a mobile imaging viewer. Automatically fed EHR data facilitates cross-department communication, including for pulmonary embolism response team (PERT) care coordination. *Based on user configuration
Clinical Trial Enrollment – AI-driven automatic patient identification for clinical trial enrollment.
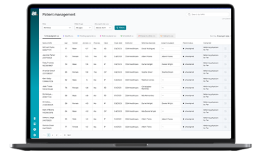
Patient Management: Identify patients needing follow-up – such as those with subacute aortic aneurysms – using integrations to track follow-up adherence, provide clinical pathway steerage and automate outreach to patients, primary care physicians or clinics.
Aidoc’s clinically validated vascular solutions automatically consolidate data, utilize AI to generate clinical insights for more effective triage and notification of vascular disease, and streamline communication to help prevent patients from being lost to follow-up, improving patient outcomes and increasing downstream procedures.



Yost, M. (2023). The Current U.S. Prevalence of Peripheral Arterial Disease. Vascular Disease Management, 20(4), 67–73. https://www.hmpgloballearningnetwork.com/site/vdm/current-us-prevalence-peripheral-arterial-disease
Worklist Reprioritization Using Artificial Intelligence Improves Turnaround Times Of Chest CT Examinations Positive For Acute Pulmonary Embolism. Harrison, B. Presented at RSNA 2021
Mechanical Thrombectomy, Artificial Intelligence and the Activation of a Pulmonary Embolism Response Team. Gupta K., Lipshutz G., Friedman O., et al., Presented at PERT Consortium, 2022
Artificial intelligence improves initial evaluation and follow-up of patients with AAA. Kostiuk et al. Yale School of Medicine, New Haven, CT, US. VAM 2024 Interactive Poster
© Copyright 2026 Aidoc
